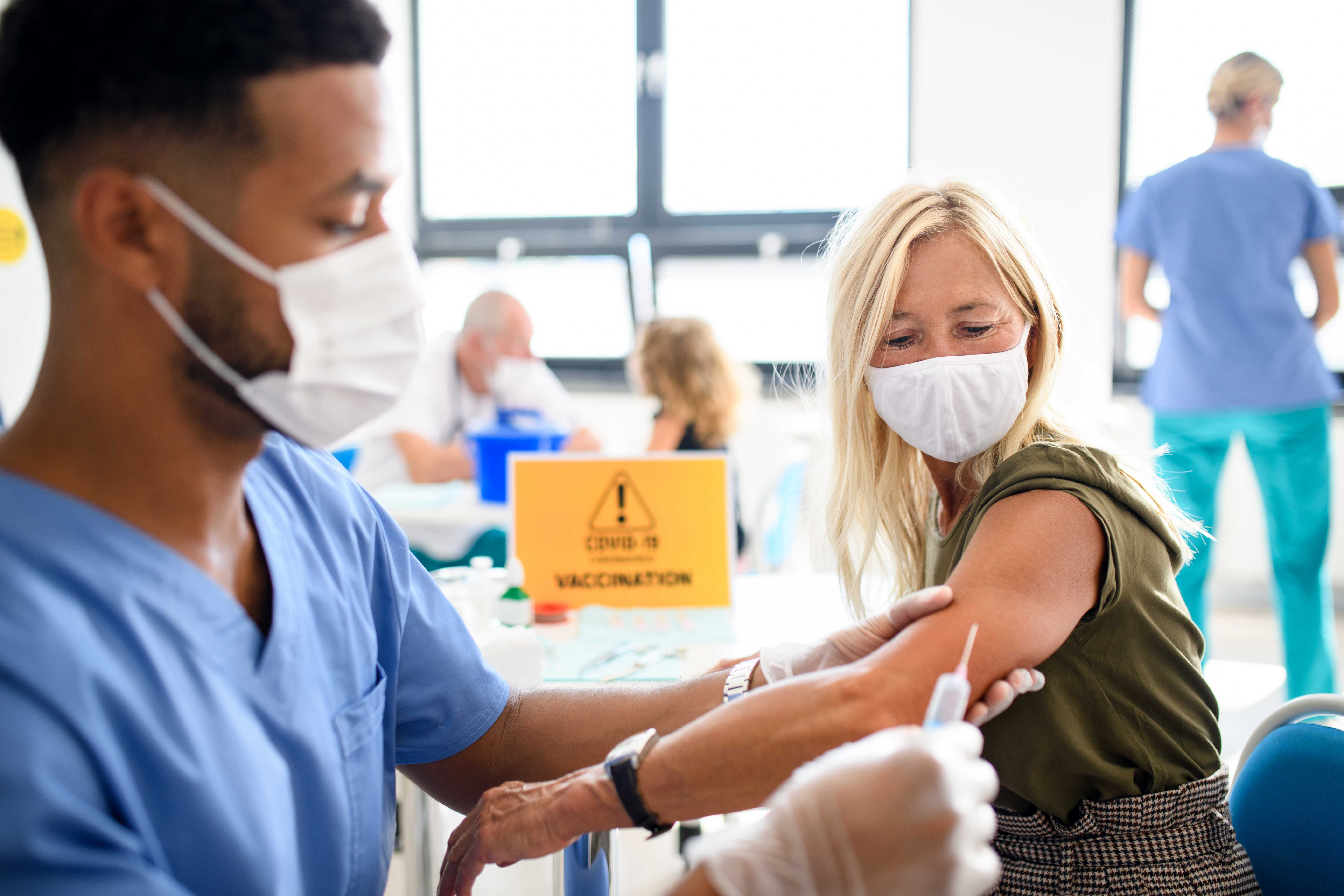
As part of Australia’s COVID-19 vaccine rollout, residential aged care providers are required to facilitate vaccination clinics within their facilities. To help aged care providers manage the process, the Department of Health has released clinical government requirements for the facilitation of COVID-19 vaccination clinics at RACFs.
In this article we summarise the key vaccination clinic requirements set by the Department of Health.
Overview
Even though you may be outsourcing the actual vaccinations to a third party, as a residential aged care provider you still have key responsibilities over the three stages of the vaccination process: preparation for the vaccine clinic, the clinic on the day, and the conclusion of each clinic and post-clinic.
Key responsibilities across these stages include:
- establishing a Clinical Lead to manage the vaccination program
- reviewing residents’ suitability to receive the vaccine
- communicating with residents and obtaining consent
- orienting residents and the immunisation provider on the day
- monitoring residents post-vaccination
- record-keeping.
Preparation for the Vaccine Clinic
Establish a Clinical Lead
You must appoint a Clinical Lead, e.g. a registered nurse, who will be responsible for managing the vaccine program at the site. The Clinical Lead’s responsibilities include:
- liaising with the Primary Health Network immunisation provider (the vaccination team)
- preparing and providing the list of residents and staff to be vaccination to the immunisation provider
- assessing the suitability of residents for a vaccine and ensuring all participants have given informed consent
- receiving a formal clinical handover from the immunisation provider at the conclusion of each clinic day.
You must give the name and contact details of your Clinical Lead to the vaccination team.
Review Residents’ Suitability to Receive the Vaccine
You must ensure your Clinical Lead assesses residents to determine if there are any concerns about their suitability to receive the vaccine. Immunisation providers should be informed of any residents that have a bleeding disorder or are taking blood-thinning medication (anticoagulant). If any concerns arise regarding resident suitability for the vaccine, the Clinical Lead should consult with the resident’s GP.
According to the Australian Technical Advisory Group on Immunisation (ATAGI), the only people who are not suitable for the vaccine are those who have had an anaphylaxis in relation to a previous dose or after exposure to any component of the COVID vaccine.
You are responsible for confirming your staff’s intention to participate (or not) in the vaccination program.
Obtain Informed Consent from Residents
Your Clinical Lead is responsible for facilitating, seeking and recording informed consent for all residents assessed as suitable to receive the vaccine. The consent should be written and stored in the Resident file for future reference.
For more information, refer to the Consent Flowchart for COVID-19 Vaccination in Residential Aged Care.
Establish Dose Requirements
Prepare a list of everyone who will be receiving the vaccine (i.e. all residents who are suitable for the vaccine and consent to vaccination).
Ensure Site Readiness
You must ensure the site is prepared in a manner that is appropriate and supports an efficient and safe vaccine clinic. This includes:
- ensuring you have a safe resident identification process in place, especially where residents are unable to state their own name and date of birth
- ensuring you are well stocked in diagnostic equipment, sphygmomanometer, oxygen saturation monitors, hand sanitizer, disinfectant wipes and other consumables
- ensuring you have PPE in stock to address any local state/territory health authority requirements.
For more information, refer to the Site Readiness Checklist.
Planning for Support of the Clinic
You must have an adequate number of appropriately qualified staff, who are familiar with and are known to the residents, rostered to support the vaccine event.
You should consider sourcing additional capability (e.g. clinical skills) or capacity, to ensure clinical safety including to facilitate and support resident flow through the clinic.
The Vaccine Clinic on the Day
Clinic Set-Up and Orientation
Your Clinical Lead must meet the immunisation provider upon arrival on-site and provide a local orientation of the facility.
Preparing Residents
You should provide the vaccine workforce with a list of residents who will be receiving the vaccine upon their arrival.
You should also provide the vaccine workforce with each resident’s consent form and information about:
- the resident’s medical conditions, allergies, bleeding disorders or immunocompromise (i.e. weakened immune system)
- any medications the resident is taking
- any reactions the resident has had to any vaccine in the past
- any communication, cultural or behavioural factors that are relevant to the vaccination process
- whether a support person is required to be with the resident at time of vaccination.
Clinic Management
You are responsible for the efficient and safe movement of residents through the clinic. You must ensure your staff use PPE in line with local state health authority requirements.
Monitoring Residents Post-Vaccination
You are clinically responsible for residents that have received the vaccine, once released from the immunisation provider’s 15-minute post vaccination observation.
You may wish to have a Registered Nurse on duty following the departure of the vaccination workforce, to manage post vaccination side effects such as fever and pain.
You should ensure you have in place clear escalation processes that staff are familiar with, and contact details for residents easily accessible, in the case of adverse events.
The Conclusion of Each Vaccine Clinic and Post-Clinic
Clinic Closure and Handover
At the conclusion of each clinic day, you will assume clinical responsibility of all residents prior to the departure of the vaccination team through a formal clinical handover with the immunisation provider. This may include a signed verification handover.
Resident Records
You must record the vaccination in each resident’s records.
Conclusion
Clinical governance is covered under Standard 8: Organisational Governance of the Aged Care Quality Standards. Clinical governance has three core areas of purpose:
- safe provision of care
- appropriateness of care, or evidence-based care
- effectiveness of care, which includes evaluation across all parts of care, underpinned by meaningful partnerships between consumers and healthcare providers.
As the gatekeeper’ to the COVID-19 vaccine for your residents, ensuring you meet the clinical governance requirements for facilitating vaccination clinics at your facility is fundamental to keeping your residents safe from harm and meeting your compliance requirements.
ABOUT THE AUTHORS
Jenny Wang
Jenny is the Content Integration Team Leader at CompliSpace and a legal research assistant for the aged care team. She has a Bachelor of Science (Financial Mathematics and Statistics) and is currently completing her Bachelor of Laws at the University of Sydney.
Mark Bryan
Mark is a Legal Research Consultant at CompliSpace and the editor for ACE. Mark has worked as a Legal Policy Officer for the Commonwealth Attorney-General’s Department and the NSW Department of Justice. He also spent three years as lead editor for the private sessions narratives team at the Royal Commission into Institutional Responses to Child Sexual Abuse. Mark holds a bachelor’s degree in Arts/Law from the Australian National University with First Class Honours in Law, a Graduate Diploma in Writing from UTS and a Graduate Certificate in Film Directing from the Australian Film Television and Radio School.